Pelvic Pain: Causes, Symptoms, Diagnosis, and Relief in Abu Dhabi
Pelvic pain is any pain felt in the lower abdomen or pelvic region. It can be sharp, dull, constant, or occasional, and may interfere with your daily routine or overall well-being. Because pelvic pain has many possible causes, it’s important to understand your symptoms and seek early medical advice.
What Is Pelvic Pain?
Pelvic pain refers to discomfort or aching below the belly button and between the hips. The pain may be short-term or ongoing and can be linked to menstrual cycles, urinary or digestive issues, or reproductive system health.
How Common Is Pelvic Pain?
Endometriosis lesions are classified into three major groups: superficial peritoneal lesions, cystic lesions on ovaries, and deep subperitoneal lesions.
A Frequent Women’s Health Concern
About 15–20% of women will have ongoing pelvic pain that lasts more than 6 months.
How Many Women Experience Pelvic Pain?
Not all pelvic pain is related to gynecology; it can be caused by bladder, gut, or even musculoskeletal issues.
Is Pelvic Pain Normal?
Early diagnosis and a tailored treatment plan help most women manage symptoms and avoid complications.
Types of Pelvic Pain
Acute pelvic pain: Sudden and severe pain, often requiring urgent medical attention.
Chronic pelvic pain: Lasts at least 6 months, may come and go, and can be complex to treat.
Cyclic pelvic pain: Occurs in patterns connected to the menstrual cycle.
Image suggestion: Flow chart or icons showing three types (bolt for acute, repeating arrow for chronic, calendar for cyclic).
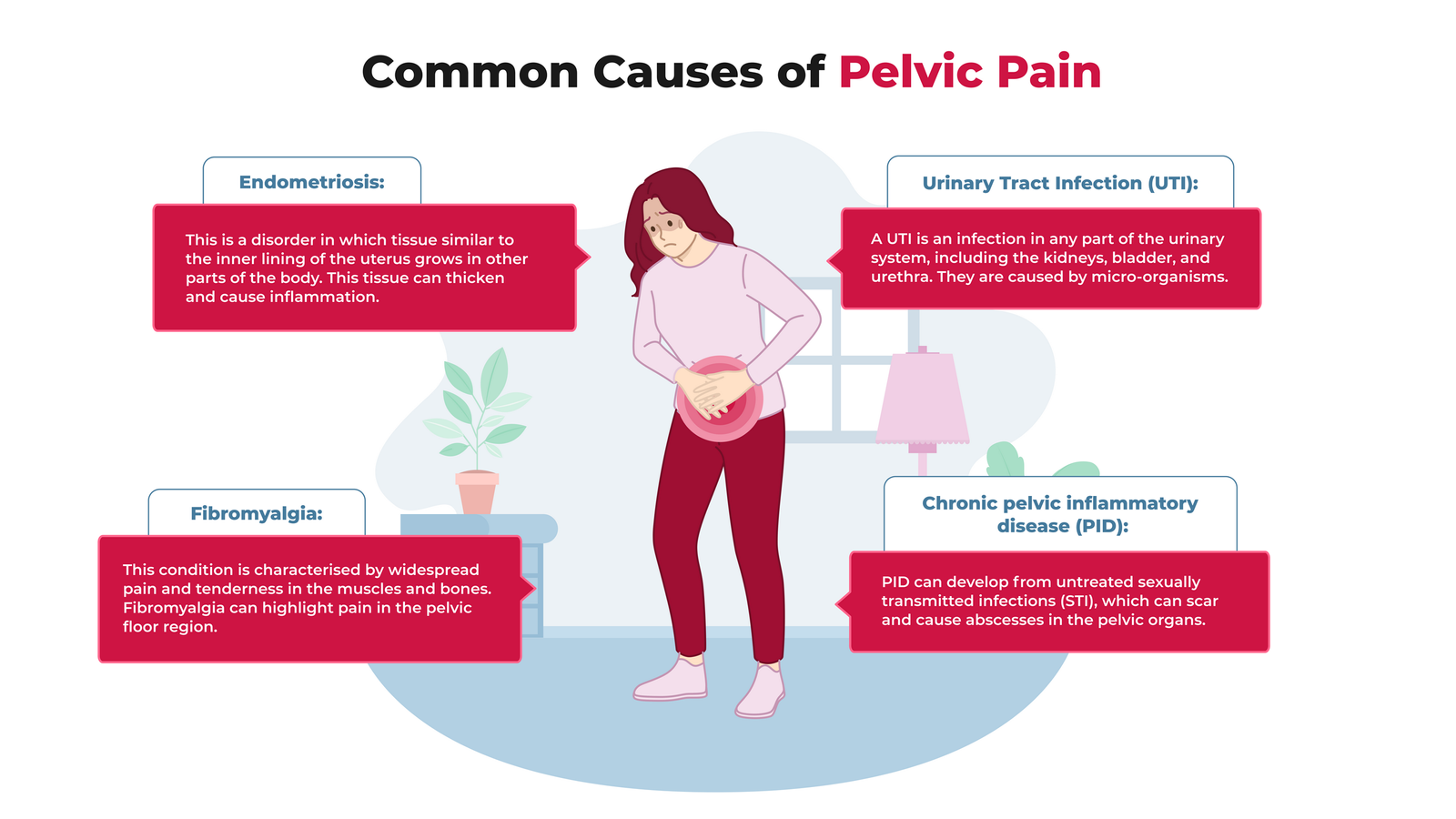
Common Gynecological Causes
Menstrual cramps (dysmenorrhea)
Endometriosis
Ovarian cysts or ruptured cysts
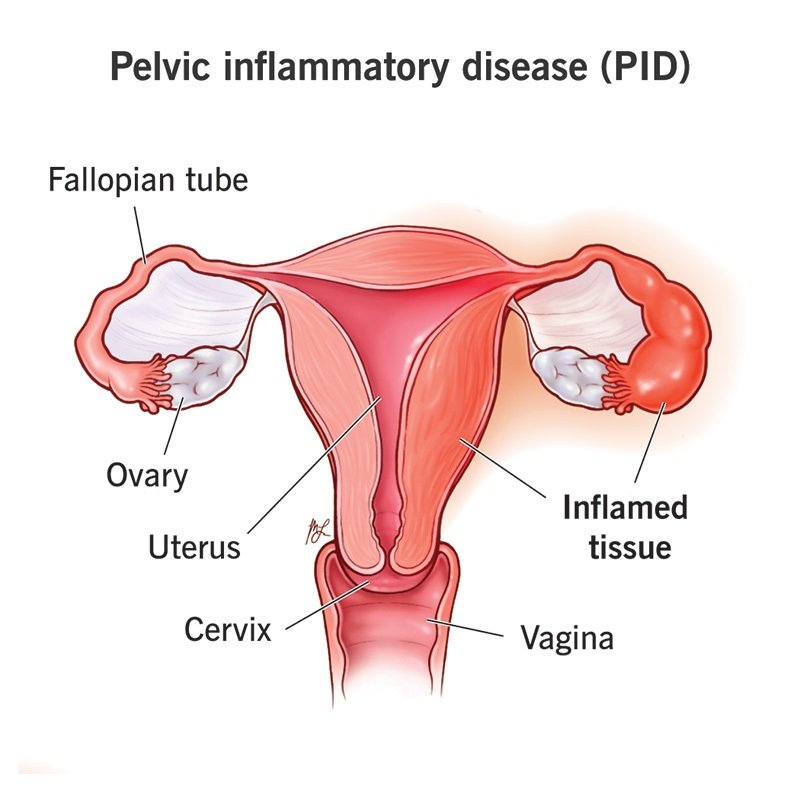
Pelvic inflammatory disease (PID)
Uterine fibroids
Adenomyosis
Ectopic pregnancy
Painful ovulation (mittelschmerz)
Pelvic organ prolapse
When Should You See a Gynecologist?
Get medical advice if you experience:
Pain disrupting daily life
Pain during or after sex
Severe or worsening period pain
Pain with urination or bowel movements
Irregular vaginal bleeding
Fever or abnormal vaginal discharge
Difficulty getting pregnant
Early evaluation can help prevent complications and provide effective relief.
How Is Pelvic Pain Diagnosed?
Your gynecologist may recommend:
Detailed medical and menstrual history review
Physical and pelvic examination
Pelvic ultrasound or MRI imaging
Blood and urine tests
Laparoscopy for definitive diagnosis (especially for endometriosis)
Treatment Options
Management depends on the cause and severity:
Pain relief: Anti-inflammatories or prescription medications
Hormonal therapy: Especially for endometriosis or fibroids
Antibiotics: For infections like PID
Pelvic physiotherapy: For chronic, musculoskeletal pain
Surgery: Laparoscopy for cysts, fibroids, or severe endometriosis
Lifestyle support: Stress management, healthy diet, gentle exercise
Chronic pelvic pain often needs a multidisciplinary approach for lasting results.
You don’t have to live with pelvic pain. With timely evaluation and personalized care, most women find significant relief—regaining both comfort and quality of life. If you’re experiencing pelvic discomfort, reach out to a gynecologist for expert support.